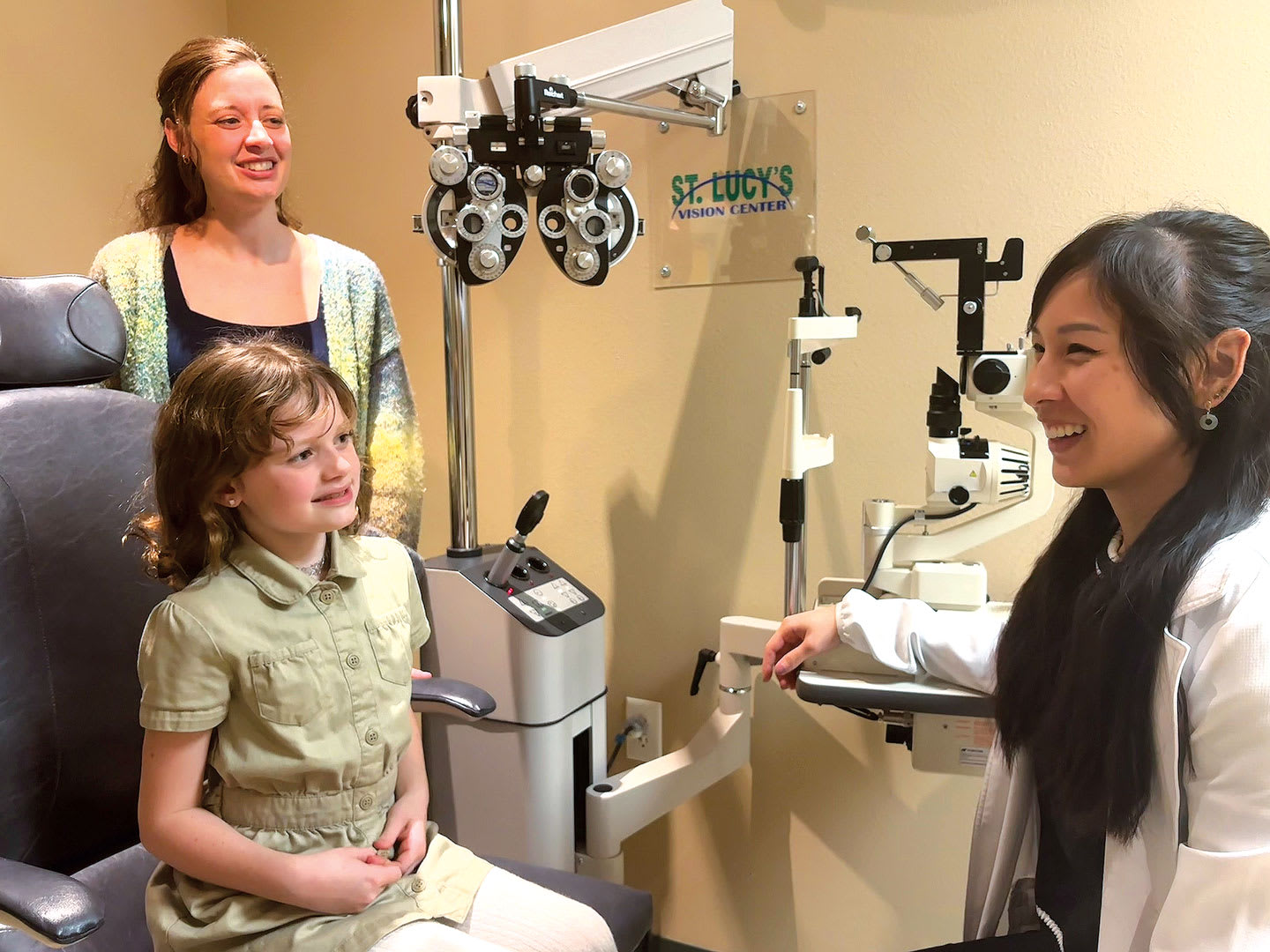
It usually starts with a question: “Doctor, did her prescription go up again? Already?” It isn’t panic in their voice, not yet. But it’s getting close.
And there it is, the moment when everything you know about refractive error, axial length, and visual development must pass through a narrow doorway: a parent’s heart. What they’re really asking is something much bigger: Is she going to be okay? Can we do anything? Should we have done something sooner?
That’s the weight of the myopia conversation. The one where science meets worry, and where what you say and how you say it can shape a child’s lifelong relationship with their vision.
To be clear, this is not a sales pitch, and it’s not a lecture. It’s an act of trust and partnership. At its best, it begins a shared journey.
Where We Usually Go Wrong
We overeducate and undertranslate. We toss out phrases like “pathologic myopia” or “axial elongation,” and then wonder why the parent’s nod starts to look eerily similar to the one they give when pretending to understand their kid’s Minecraft or Roblox tutorial.
Informed consent isn’t just a signature on a form, it’s a conversation. It’s informed understanding. It’s meeting families where they are and guiding them, not pressuring them, toward a decision that honors both their concerns and their hopes.
How Do You Do It?
Start with the human stuff, set in a framework: what we see, what it means, and what we can do next. Three sentences. Clear language. Try it like this: “Your daughter’s eyes are changing faster than we’d expect for her age. That matters because faster change increases her chances of needing thicker glasses and facing more serious vision problems in the future. The good news is we have safe ways to help slow it down, and we can choose an option that fits your family.”
Then pause, because questions come after oxygen, and trust grows in the pause. Watch their eyes. Match their pace. If they get quiet, let the quiet do its work. Then ask, “Does that make sense so far?” When helpful, I relate the child’s progression against family history or demonstrate blur with trial lenses. When we’re on the same page, we take the next step.
That’s Your Cue to Talk Options
The options should not be listed out like the menu at your favorite fusion restaurant but offered in conversation. For example: “Some families like the idea of overnight lenses that reshape the eye while they sleep. Others prefer daily contact lenses or eye drops that gently slow the change. Let’s talk about what might fit best for you and Ava.”
Ask questions. Listen deeply. This isn’t about selling a modality. It’s about giving a family the dignity of choice, wrapped in your best guidance.
And when they say yes? It’s not just yes to a product. It’s yes to you. To your care. To your commitment. And yes, to a shared belief that their child’s future is worth the effort.
The myopia conversation isn’t always easy. But it may be one of the most meaningful you’ll have in practice. It’s where clinical excellence meets humanity. And I’ve found that when we lean into it with honesty, hope, and just a hint of humor, everyone sees a little more clearly.
Even you. Especially you. OM